Combining BFR rehabilitation with neuromuscular electrical stimulation holds quite a bit of potential in the healthcare arena. Read the findings of some studies that have been conducted to gain more insight. Neuromuscular electrical stimulation (NMES) has long been used to aid recovery and maintenance of size and strength following surgical procedures and other injuries impairing neuromuscular function. However, it’s utility is limited by our physiology and tolerance to the procedure. Therefore, if personalized blood flow restriction can enhance NMES’s ability to create muscle adaptation, that would equate to significant value for our clients in this evolving healthcare market.
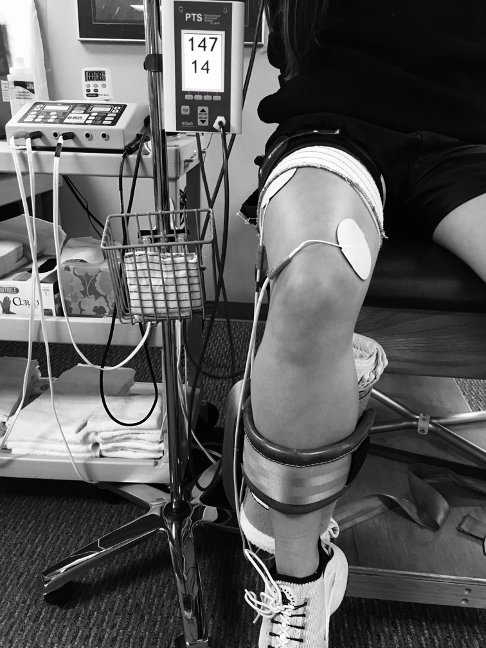
This is a review of three studies that have examined three different questions regarding NMES’s use in combination with BFR. Inagaki (2010) demonstrated the ability of NMES + BFR to increase serum GH at a low level of stimulation. They used NMES at 20% of MVC for knee extension, with and without BFR applied to the proximal thigh at 150 mmHg. Ultimately their main research goal was to examine whether or not there is a local metaboreflex vs. centrally mediated control of GH secretion. Their findings demonstrated that there does seem to be a metaboreflex, triggered by lactate build up within the exercised muscle involved in GH secretion from the pituitary. This indicates that we, as clinicians, can achieve an environment within the muscle for our clients that may play a role in their healing, and recovery of size and strength even when their exercise tasks are limited by precaution, pain, or tolerance to the NMES modality.
| Growth Hormone (ng/mL) | Pre | 2 min | 15 min | 30 min |
| NMES w/ BFR | NO CHANGE | NO CHANGE | INCREASE | INCREASE |
| NMES w/o BFR | NO CHANGE | NO CHANGE | NO CHANGE | NO CHANGE |
Gorgey (2016) published a fascinating study using NMES + BFR on incomplete spinal cord injury patients. They sought to determine if they could improve size, strength, and function of the all important wrist extensors via NMES + BFR; thus amplifying, or reproducing without load, results that have already been demonstrated using NMES alone. After six weeks of training, the NMES + BFR group did, in fact, add more muscle size and strength, than the NMES group. The functional increases were similar between groups for “grasp and release” of a soda can, block, weight, and fork, but the BFR group did improve the speed with which it was able to grasp and release a peg. The authors cite many limitations that give them pause in the interpretation of their results but, nonetheless, were confident in claiming that the combination of NMES + BFR demonstrated its potential to achieve desired results without the challenge of externally loading wrist extensors in the SCI population. Another aspect of the Gorgey study examined flow-mediated dilation of the NMES + BFR group vs. BFR alone. What they found was that the acute dilation of the upper extremity vasculature was amplified in the NMES group vs. the BFR alone group. Presumably, the accumulation of metabolites in the NMES group aided the resultant dilation upon release of the occlusion. The authors conclude that this finding may provide evidence to support a potential contribution of lactate accumulation and nitric oxide release in the role of skeletal muscle hypertrophy.
Natsume (2015) sought to examine NMES + BFR’s ability to increase muscle size, isometric, and isokinetic strength. Part of the problem they sought to address is the fact that NMES’s ability to create muscle adaptation is directly proportionate to the intensity of the NMES used. They cite a variance in tolerance from 12-95% of maximal strength. Subjects underwent twice daily isometric knee extension exercise bouts, five days a week for two weeks, with or without BFR using NMES at a 5-10% intensity of maximal strength. In addition to examining the training period’s outcomes, they assessed the groups after a 2-week detraining period. The NMES + BFR group showed significant improvement in muscle size and strength compared to NMES alone. However, these results were only partially maintained during a detraining period.
| size | isom | 90° / s | 180° / s | |
| NMES + BFR | 3.9% INCREASE | 14.2% INCREASE | 7% INCREASE | 8.3% INCREASE |
| NMES | NO CHANGE | NO CHANGE | NO CHANGE | NO CHANGE |
| BFR detrain | 3.0% DECREASE | 6.8% DECREASE | 1.9% DECREASE | 0.6% DECREASE |
In summary, we have evidence to indicate that combining low-intensity BFR with NMES can increase muscle size and strength in healthy and neurologically impaired populations, as well as positively affect blood flow to the exercised region. Due to the low-intensity, the intervention may need to be performed for longer bouts and/or with higher frequency to see adaptation. There hasn’t been a study yet to show the effects of BFR with NMES 2-3 days a week in an injured or post-surgical population, but the clinical results are very promising. This can be a very valuable tool for maximizing muscle activation and minimizing loss when mechanical loading is limited.
Thank you, Kyle Kimbrell, MPT for the article summary.


