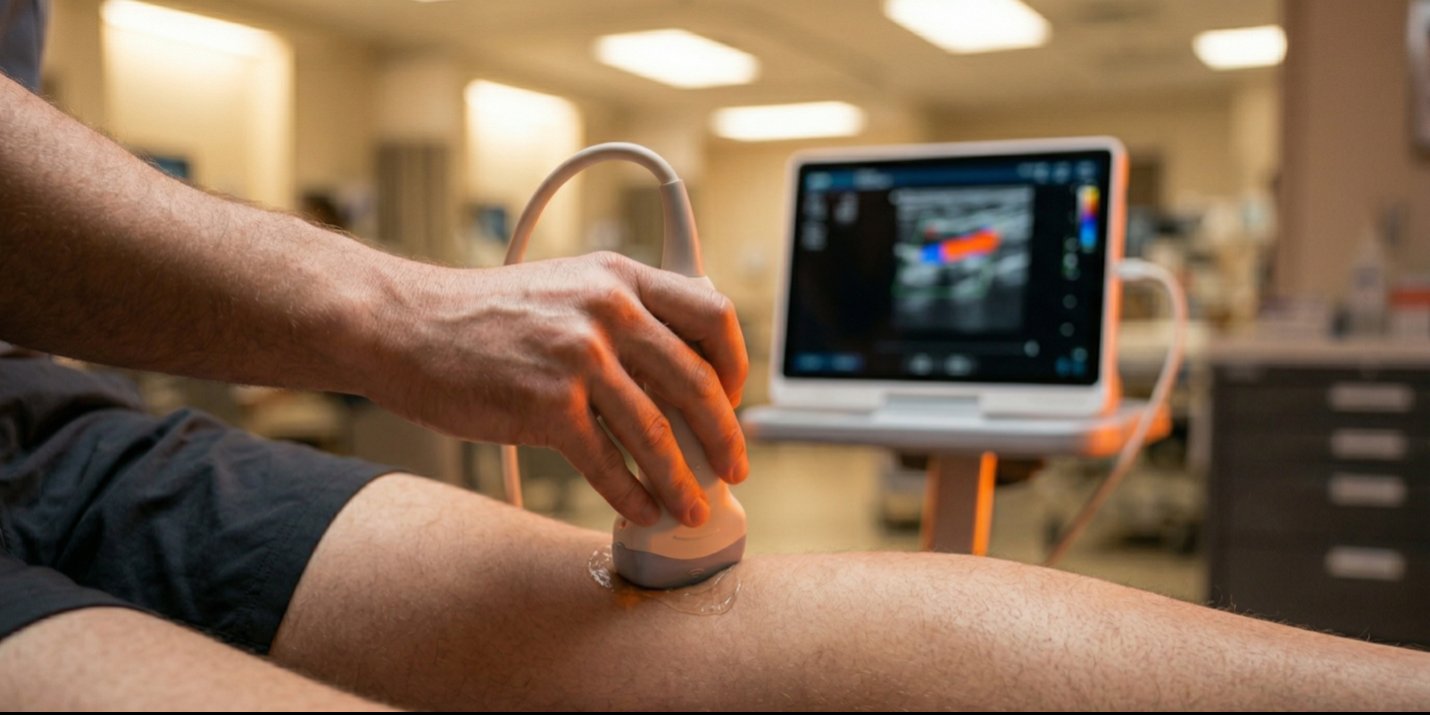
A woman walks into a rural emergency department in Arizona with posterior knee pain following a minor car accident five days earlier. Classic presentation: step on the brake, twist through the knee, probable meniscal injury. Her Wells criteria score? Negative one. No swelling. No redness. Zero clinical suspicion of a blood clot.
But John Van Eyk, a physical therapist embedded full-time in the ED at a 52-bed hospital on the Navajo reservation in Fort Defiance, Arizona, did something most clinicians in his position wouldn’t have done. He pulled out an ultrasound probe.
The Case That Changed Everything
John had taken Steven Ramsey’s point-of-care ultrasound (POCUS) course the previous summer. One principle stuck with him above all others: always check the neurovascular bundle. It’s right there. It takes seconds. Just check it.
So when he positioned the probe over the posterior knee to look for the Baker’s cyst he expected, the neurovascular bundle appeared first on screen — and it was huge. He tried to compress the vein. It wouldn’t compress. He repositioned the patient. Still wouldn’t compress.
John called the physician. Within minutes, a confirmatory duplex ultrasound confirmed what he already knew: a significant DVT that every standard clinical screening tool had missed.
“Within 30 seconds of the probe on there, I found evidence of the DVT. Her Wells criteria was negative one. There was no reason to suspect this.” — John Van Eyk, PT |
Why This Matters Beyond One Patient
A DVT alone won’t kill a patient. A pulmonary embolism will. And if that clot had gone undetected — if John had simply performed manual techniques and sent her home — the outcome could have been catastrophic.
The science backs up why this approach works. Two-point compression ultrasound (checking at the groin and behind the knee) maintains sensitivity and specificity above 90% for detecting DVTs. The exam takes two to five minutes. The skill to perform a basic vascular screen can be learned in a weekend course and refined through clinical practice.
As Steven Ramsey explains, the only real gap in a limited compression exam is the mid-femoral region, which accounts for roughly 5–7% of all DVTs. Adding that compression site adds minimal time to what is already one of the fastest diagnostic screens available to a rehab clinician.
From Weekend Course to Daily Clinical Tool
John didn’t take one course and shelve the skills. He uses ultrasound two to three times per day across eight to ten patient encounters. In a setting where emergent MRIs aren’t an option for musculoskeletal injuries and where he serves as a de facto primary care provider triaging patients across fast-track, main ER, observation, and rapid triage, ultrasound has become indispensable.
He’s used it to identify a growth plate fracture before the X-ray could be pulled up, diagnose intersection syndrome in a wrist when the nearest diagnostic ultrasound facility was hours away, and screen cardiac and pulmonary presentations alongside the emergency physicians.
“Probably the most important course I’ve taken as a PT, honestly. It didn’t just teach me a skill — it gave me the ability to look into somebody’s joint and make an early diagnosis.” — John Van Eyk, PT |
Credibility That Compounds
One of the most powerful outcomes John describes isn’t a clinical finding — it’s what happened after. The physician who ordered the confirmatory scan didn’t need to see the ultrasound herself. Her response: “If you think there’s a DVT there, there’s probably a DVT there.”
That level of interdisciplinary trust doesn’t come from a credential alone. It comes from consistent, competent use of a diagnostic tool that physicians respect. And now, when John requests any confirmatory ultrasound, nobody argues.
John is now pursuing his RMSK (Registered Musculoskeletal Sonographer) certification — the same credential physicians earn, negotiated for physical therapists through the APTA. Steven Ramsey is planning to sit for the RDCS (cardiac equivalent) to help open that path for the profession as well.
What’s Coming from ORS
Steven Ramsey’s general POCUS course (the one John took) covers approximately 75% musculoskeletal content plus vascular, cardiac, and pulmonary fundamentals. Two new specialized courses are in development and expected to launch this year:
- Ultrasound for the Elite Athlete — designed for ATCs and PTs working with high-level athletic populations. At last year’s NBA Combine meetings, DVTs and Achilles injuries were the two hottest clinical topics discussed.
- Critical Care Ultrasound — built for PTs, OTs, and other clinicians working in ICU and acute care settings, where cardiac and pulmonary imaging becomes essential.
Both courses will be hosted through Owens Recovery Science, expanding ORS’s education platform beyond BFR for the first time — because diagnostic ultrasound and blood flow restriction share a fundamental connection through vascular safety screening.
Ready to Add Ultrasound to Your Clinical Toolkit?Explore Steven Ramsey’s POCUS courses and all ORS education offerings. |
Listen to the full episode on YouTube or wherever you get your podcasts.